
Endometriosis happens when tissue similar to the uterus lining grows outside the uterus. This tissue can show up on the ovaries, fallopian tubes, and other organs in the pelvis. When you get diagnosed with endometriosis, your doctor might mention a stage number. Knowing what these stages mean helps you make better choices about your treatment.

Doctors use a system from the American Society of Reproductive Medicine to classify endometriosis into four stages. The stages go from stage 1 (minimal) to stage 4 (severe). These stages come from what doctors see during surgery, not how much pain you feel. The staging system uses points. Doctors look at how many tissue growths you have, where they are, how deep they go, and how much scar tissue there is. A score of 1-5 points indicates stage 1 endometriosis. A score above 40 points means stage 4 endometriosis. The stage doesn't tell you everything about your symptoms. You could have stage 1 and feel terrible pain. Someone with stage 4 might feel little discomfort. The endometriosis severity from staging shows what the disease looks like, not how it feels.
Stage 1 endometriosis is called minimal endometriosis. At this stage, you have a few small, shallow tissue growths on the surface of the tissues. They look like tiny spots or patches on your pelvis or abdominal lining. There's little or no scar tissue.
But mild on paper doesn't mean mild symptoms. Many people with stage 1 endometriosis have serious endometriosis pain. Women with stage 1 can have trouble getting pregnant. Even minimal endometriosis can hurt egg quality or cause inflammation.
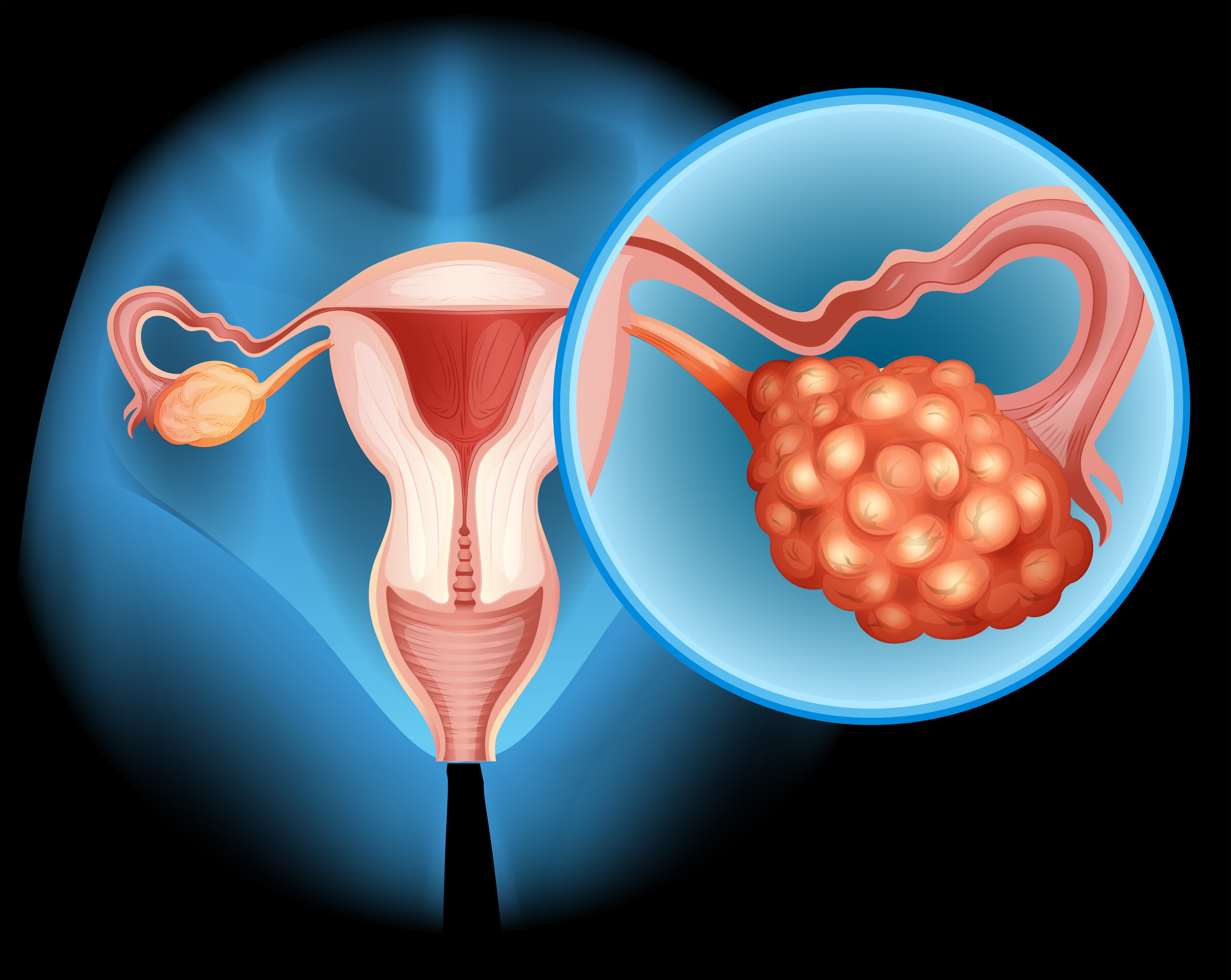
Stage 4 endometriosis is the most severe stage. You have many deep tissue growths in the pelvic area that dig into organs like the ovaries, fallopian tubes, bowel, and bladder.
Stage 4 often has large ovarian cysts called endometriomas or chocolate cysts, named for the dark brown blood inside them. Another big problem is thick scar tissue called adhesions. These bands stick organs together. In bad cases, frozen pelvis happens when all pelvic organs get bound together by thick adhesions.
The deep implants and adhesions often cause serious fertility problems. Yet some women with stage 4 feel little pain or no symptoms at all.
The main differences come down to how much tissue there is and where it grows.
Number of implants: Stage 1 has a few small growths. Stage 4 has many implants spread through the pelvic area.
Depth: In stage 1, tissue sits on organ surfaces. In stage 4, tissue digs deep into organs and can grow through the walls of the bowel.
Scar tissue: Stage 1 has little to no adhesions. Stage 4 has thick, dense scar tissue bands that bind organs together.
Cysts: Ovarian cysts are rare in stage 1. Large endometriomas are common in stage 4.
Surgery difficulty: Removing tissue in stage 1 is usually simple. Stage 4 needs complex surgery by specialists.
.jpg)
Pain is a common symptom of endometriosis, but pain levels don't match the stage. Research shows that endometriosis pain has little connection to staging. Someone with stage 1 might have bad pain during their period. Someone with stage 4 might have mild cramps or no pain. Where tissue matters more than how much there is. Small implants might press on nerves and cause intense pain. Large cysts might not hit sensitive areas.
Common pain symptoms are painful period cramps that get worse over time, ongoing pelvic pain, pain during or after sex, pain when going to the bathroom during your period, and lower back or belly pain. Some people get digestive symptoms like bloating, nausea, constipation, or diarrhea during their period.
The only sure way to diagnose endometriosis and find its stage is through surgery called laparoscopy. During this procedure, a surgeon makes small cuts in your belly and puts in a tiny camera to view the pelvic organs and look for endometrial tissue.
Before surgery, your doctor will do a pelvic exam to feel for cysts or scar tissue and might order an ultrasound to look for ovarian cysts. These tests can point to endometriosis, but can't confirm it or tell you the stage. Getting diagnosed takes time for many women, about seven to ten years from when symptoms start.
Whether you have stage 1 or stage 4, endometriosis can affect your whole life. Finding good medical care matters. Look for a doctor who listens to you and takes your pain seriously.
Support groups, tracking your symptoms in a diary, and taking care of your mental health all help. About 1 in 10 women of childbearing age has endometriosis. With the right treatment and support, most women with endometriosis can handle their symptoms and live full, active lives.


Symptoms don't reliably differ between stages. Both can cause severe pain, heavy periods, and painful sex. Some women with stage 1 have terrible symptoms while others with stage 4 have none. Where implants are matters more than how many. Stage 4 more often causes digestive problems from bowel involvement and fertility trouble from scarring and large ovarian cysts.

Yes, but you can't predict progression. Endometriosis doesn't always move through stages in order. Some women stay at the same stage for years, others get worse, and some improve. Research shows little evidence about progression rates. Early treatment may help prevent worsening and protect fertility, which is why doctors often suggest treating even minimal disease.

The definite method is laparoscopy, a surgery where doctors put a camera through small belly cuts to view pelvic organs. They find implants, take tissue samples, and assign a stage. Before surgery, doctors use pelvic exams and ultrasounds, but these can't confirm endometriosis. Diagnosis often takes seven to ten years because imaging misses small implants.

Not always, though doctors usually recommend it. If pain is okay with medication and you're not trying to get pregnant, surgery might be put off. But large cysts, blocked tubes, or bowel and bladder involvement usually need surgical removal. Stage 4 surgery is complex and needs endometriosis specialists. After surgery, hormone therapy helps prevent it coming back. Some manage with hormones alone if surgery is too risky.